 Shivana Anand and Rebecca Northover highlight the signs that better classify caries risk in paediatric patients.
Shivana Anand and Rebecca Northover highlight the signs that better classify caries risk in paediatric patients.
Risk assessing paediatric patients is of utmost importance in this day and age. The rise of caries within the younger population is at a staggering high and the number of children being admitted for extractions under general anaesthesia has peaked and is continuing to do so. Tooth extractions are amongst the top causes for hospital admittance of children between the ages of five and nine.
As general dental practitioners we need to look out for signs that better classify the caries risk of our paediatric patients. A holistic approach needs to be taken and this is a prime example of how the examination truly starts in the waiting room and not just limited to the intraoral assessment.
So what should we be looking out for?
Complaints
Before beginning a paediatric examination, it is imperative to gain a history of any dental pain, swelling, or disruption to a child’s day-to-day life that may be attributed to their teeth. Usually the child can point to the area causing concern or the parent can indicate what side of the mouth the child has been holding when in pain.
Parents often state that dental pain affects their child’s performance at school, their sleep and their ability to eat. Any of these is a large cause for concern.
A common telltale sign that a parent may talk of is a ‘gum boil’ that can appear and disappear adjacent to the tooth. These classic examples should be an indication that a tooth may need pulp therapy or even an extraction.
History of complaints
Assess the patient’s notes before their arrival. It is beneficial to see what teeth may be of relevance and possibly associated with the pain on presentation; have a look through any history of complaints previously or treatment carried out.
Social history
Diet history
A diet history is key to gaining an insight into a child’s lifestyle. Asking the child questions about their favourite drinks and foods and what they normally snack on is a good start. Try to ask open questions to allow the child to start talking more. Ask them to describe a usual day of food consumption. Speak to the parents to gain an insight into foods and drinks that their child enjoys and what they usually eat for breakfast, lunch and dinner.
School lunch is a good area to explore. Do they have a school lunch or is it packed? This can determine whether their food intake is controlled – if it is then at least parents can input what their child is and is not eating.
Ensure you explain why you are asking these questions and share your rationale to prevent parents feeling interrogated. If parents understand a team effort is required they usually appreciate feeling included.
Children who are deemed at higher risk should be asked to complete a diet diary. Three consecutive days including at least one weekend day is the ideal. This gives you a good outlook on school life versus home life. Look out for:
- Frequency of sugar containing food and drink
- Quantity of sugars in particular foods
- Children who are poor eaters, that may cause parents to compensate for quantity by allowing frequent snacking to maintain the child’s calorie levels
- Sugar trends within the child’s diet.
When the patient returns for their review appointment ensure you use this diet diary as a tool in making the family see where lifestyle changes can be made. Let them co-diagnose what the problems are and circle foods to be aware of.
Ensure that you allow families to understand that there are alternatives that can be explored for most high-sugar foods. Aim to give suggestions for improving the child’s diet and listen to any concerns that the family have. Be a supportive healthcare professional and not a judgmental one.
Sibling history
This is a really important aspect of the history. If you treat one child, you will likely be treating their siblings too. Know the background of the family – see what trends occur within their diet, lifestyle, beliefs, education and socio-economic backgrounds.
In most cases these are the differentiating factors between low- and high-risk children. Children with siblings who have suffered from caries are more likely to also suffer from the same disease.
The number of children being admitted for extractions under general anaesthesia has peaked
In these families you need to have faith in your oral hygiene education and ability to make lasting change. You can deliver priceless healthcare here and have an effect on the whole family. If you do not believe us, then try it with the eldest sibling – really commit to making that lasting change in their lifestyle.
Everything from oral hygiene, fluoride beliefs, diet analysis and education of dentistry should be discussed. In these cases, you will hopefully see that the preventive advice given for the older sibling was understood and taken on board by the parents and put into practice for the younger siblings.
Socio-economic status
Note down which school the patient attends – check if the school has an oral hygiene programme running and if in fact a dental healthcare professional has been into the school to discuss oral hygiene instructions, provide fluoride varnish or give dietry advice. It is known that children from families of lower socio-economic status are more at risk of developing caries.
The dental aspirations of the parents will also affect the child; a positive ethos at home will be the starting point of maintaining good oral health. Parents with low dental aspirations, lack of education or having had a previous bad or traumatic dental experience are at risk of negatively impacting their child’s dental health and ideology. Try to control this sooner rather than later – it is our role to educate and assist.
Dental history
Last recall
Patients without prior exposure to dentists can cause concern. This is a multi-factorial area to understand and can be broken down to why you should be concerned at a long or unreliable recall. These are areas you should be aware of:
- Undiagnosed disease
- No maintenance plan
- Compliance from the family
- Cooperation from the child
- Potential lack of dental education.
These children may need stabilisation alongside building of rapport with the influence of parents who may also need aspects of dental education. It is important to stress at this stage to the parent the importance of integrating dental visits into a child’s life at an early age and for any younger siblings this advice could be advantageously put into practice.
Oral hygiene habits
We are all aware of the basic oral hygiene advice comprising predominately of brushing techniques and fluoride interventions and I am sure we all have our own methods of conveying these to patients.
However, be mindful that families may still have unanswered questions. It helps to have a practice information leaflet with all information written down for patients. This allows for a message parents can look back on after the original verbal discussion. It is almost impossible for all advice given in surgery to be retained later on.
Make a note of who supervises or brushes the child’s teeth, at what time of the day this happens and how often. Check if any food or drink is consumed in the evening after tooth brushing has occurred. Many children go to bed with bottles of milk and juice after brushing their teeth. In these situations, dental education is paramount and a certain degree of patience and understanding will be needed to change a set routine.
Parents with low dental aspirations, lack of education or having had a previous bad or traumatic dental experience are at risk of negatively impact their child’s dental health and ideology
Fluoride habits
Always check which toothpaste the child is using; parents can be informed where to find this information on the ingredients of toothpaste. Ensure ‘spit don’t rinse’ is explained, especially the importance of why. Be particularly wary of parents who use herbal toothpastes and who particularly object to fluoride use at all.
If parents appear confused, ask them to bring in what they use. You can then have an open and frank discussion about their options. If they are willing to change then fantastic but if they are not, making the family extremely aware of all risks associated with avoiding fluoride is paramount. Some areas are fluoridated and these populations tend to have a better control on caries.
Compliance
Compliance needs to be assessed from the waiting room. Are they stuck to mum’s hip? Do they say hello? Have they already been teary before even coming into the surgery? Be open and friendly. Ensure this is a fun experience and do not push them into doing anything they do not want to. The rapport you build with the child will definitely affect how you carry out the treatment required and the extent of which treatments can be realistically carried out. All education and healthcare advice will be lost if the child does not trust you!
Medical history
Confirm all medications with parents and whether they are sugar-free. With sugar-containing medicines, ask what time of the day they are taken and if they are taken with or without food. It is worth checking in the BNF if sugar-free options are available and if the general practitioner can change the medication; a multi-disciplinary approach is needed here.
Some parents may over-compensate with medically compromised children and so their diet may be less restricted than otherwise; this can lead to a higher influx of ‘treat-food’ that is often high in sugar. Alternatively, medically compromised patients have a completely different lifestyle that cannot be easily changed or particular foods that they cannot eat.
This of course can be a delicate subject to approach with parents. However, the child’s dental health must be put first and so diet advice in the child’s best interests is paramount to stress to parents. Work together to see what can be changed to assist the child’s dental health and what areas may need to just be minimised as much as possible within the circumstances.
Physical and intellectual disabilities may also affect children’s caries risk. Partly because they pose a greater challenge to supervising parents, but also because children with these disabilities often dislike the sensation of tooth brushing and thus refuse to allow any cleaning to take place.
Intraoral assessment
Plaque levels
Note the standard of oral hygiene as good, moderate or poor. A plaque score is an interactive way to include the child in their treatment. Tell the family the percentage of plaque present and use it as a marker for improving at each visit. This can be a fun challenge for paediatric patients who can then enjoy beating the score at each subsequent visit.
The dental aspirations of the parents will also affect the child; a positive ethos at home will be the starting point of maintaining good oral health
Note if there are any plaque modifying factors, such as orthodontic devices, calculus, loose teeth and partially erupting teeth. These can be adapted into your care plan, with an aim to reduce plaque levels for the child and improve oral health.
Calculus levels
High calculus levels are particularly found in patients who are percutaneous endoscopic gastrostomy (PEG) fed; however, in practice these patients are rarely seen and so high levels of calculus are a cause for concern. Most children will find calculus associated with their lower incisor teeth on the lingual surface. Here is the best place to start with floss or Tepe advice, as it is an easy location to practise and from six years old most children will have these incisors. Again, educate and put a plan into action.
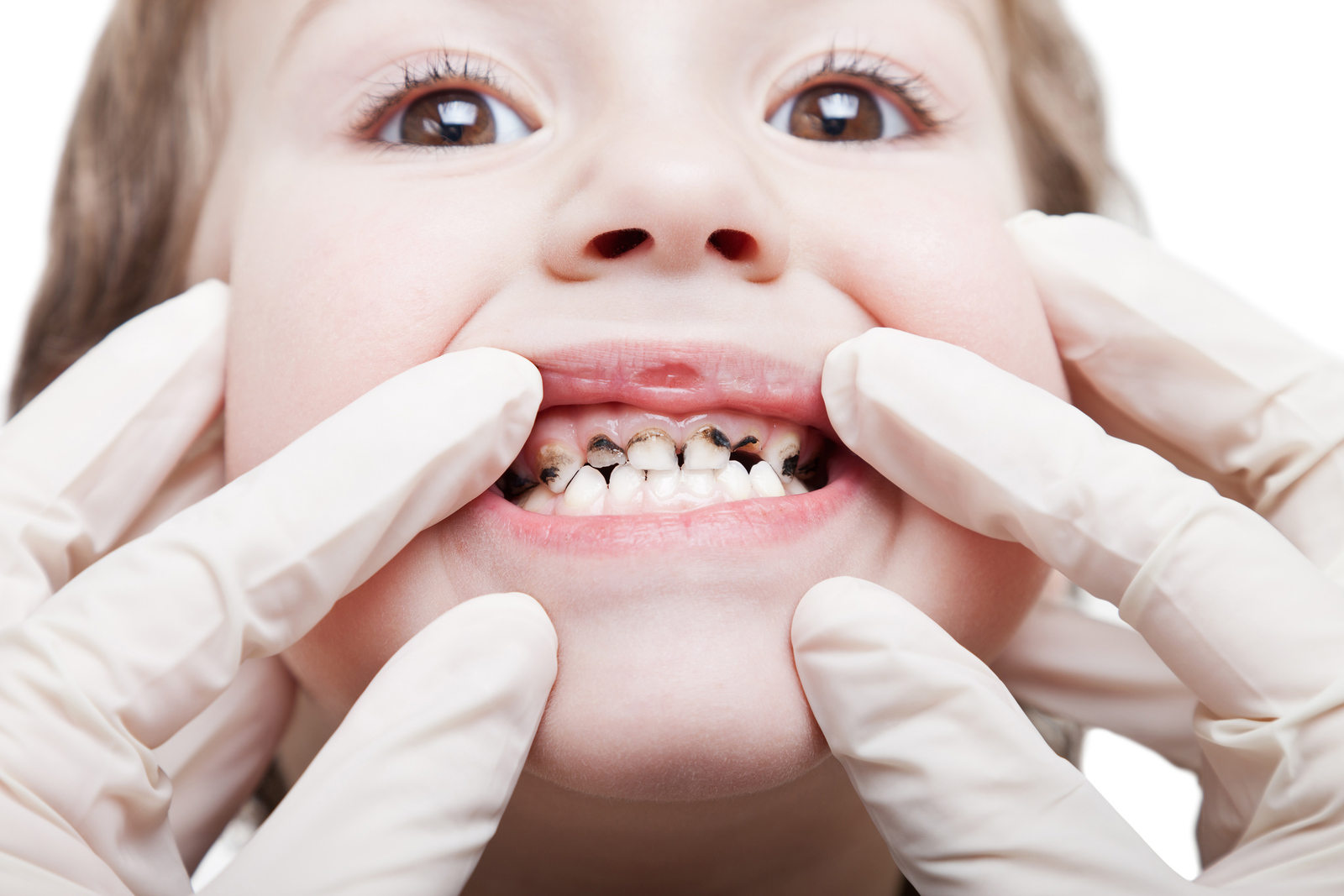
Carious lesions
Note all active or arrested lesions. Arrested lesions show a previous high caries rate in which either diet or oral health has improved. These children should still be monitored closely as they could still slip back into a high-risk category. Early extraction sites need to be noted as this is usually due to previously carious teeth that were unrestorable.
Previous restorations – composites, amalgams and metal preformed crowns – need to be monitored and caries status needs to be checked with radiographs on these teeth.
Risk status
Overall risk status comes from every part of information gathering you have compiled throughout the patient journey. The definition for high caries risk is >2 new carious lesions within the past 24 months. Low caries risk is a child who gives little concern for developing dental disease. Medium risk patients may be those slipping upwards from a low risk group or those improving from high risk. There is not always a set standard as to how to categorise children and a certain level of clinical experience and judgement is required.
However, keep an open mind. A child who has undergone multiple extractions, stainless steel crowns all under general anaesthesia, but now has no current caries. Would you be happy to see them every two years? Would you still want to apply fluoride at every visit? View the patient as a whole including past dental history and ensure you tailor each care plan to their specific needs as well.
Rebecca graduated from King’s College London in 2014 and went on to complete her vocational training in Bristol. She has completed a dental core training post in paediatric dentistry at St Thomas’ Hospital and is currently undertaking a dental core training post in restorative dentistry at Guy’s Hospital. Rebecca has completed examinations for membership of the Joint Dental Faculties of the Royal College of Surgeons of England.
Shivana Anand is a King’s College London newly qualified dentist. She is currently doing her dental core training at UCLH and The Eastman in maxillofacial and oral surgery. She also works at Harley St Dental Studio part time. Shivana enjoys her role as an honorary tutor at Guy’s Hospital. She is the co-founder of Dental Training Consultants, which is a group that organises courses for undergraduates to aid in their dental foundation interviews.


