Dominic Hassall discusses the difference between screw and cement retained restorations.
Complications may arise in the surgical phase of implant treatment with failure of integration or damage to vital structures, or there may also be late complications that are either mechanical or biological (including aesthetic).
A full assessment of the medical history and dental condition should be undertaken to identify risk factors such as smoking, periodontal disease, poor oral hygiene and parafunction. There are emerging potential risk factors such as rheumatoid arthritis and alcohol consumption.
As implants lack proprioception and the shock absorbency of a periodontal ligament, it should be no surprise that mechanical complications occur, current literature also indicates peri-implantitis to be a significant condition.
Complications
Mechanical complications may include:
- Abutment screw loosening/fracture
- Abutment fracture
- Framework fracture
- Fracture or premature wear of aesthetic veneering material.
Biological complications may include:
- Gingival overgrowth
- Mucositis
- Peri-implantitis.
There may also be aesthetic complications where the patient is disappointed with the final aesthetic result and requests changes or the prosthesis may need to be removed and adjusted for easier oral hygiene.
Materials
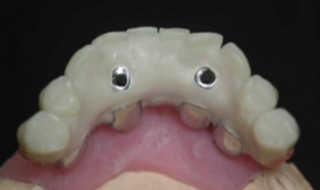
Although cement restorations function well they should not be considered the first choice, particularly for patients where risk factors have been identified due to the difficulty with restoration removal when permanent cements are used. Temporary cements allow restoration loss at inconvenient times for the patient. Care must also be taken when removing subgingival cement that has been implicated in peri-implantitis.
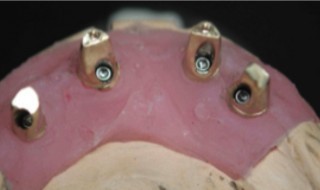
Screw fixation with the Bredent screw fixation system allows a temporary cement to be used but with the security for the patient of additional screw retention (Figures 1 and 2).
In the anterior maxilla, facially inclined implant angulation can complicate screw-retained restorations with the screw access hole being facially placed or on the incisal edge.
A number of solutions to this problem exist, which also have documented passive fit, including:
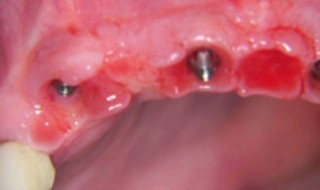
- Cresco (Dentsply Implants) (Figures 3 and 4)
- Atlantis Isus (Dentsply Implants) (Figure 5)
- Cara (Heareus Kulzer) (Figure 6).
The Cresco system uses an intermediate uni-abutment, bendable screw access tube and slot screw to locate access palatally.
Both the Cara and Atlantis systems allow the screw access to be located more palatally with novel screw and driver designs and CAD/CAM technology.
Clinical examples
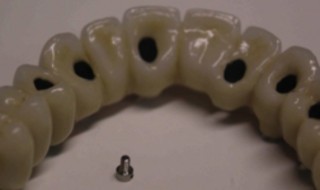
The first case demonstrates a Cresco bridge that developed gingival overgrowth after three years as the patient commenced blood pressure medication, which induced gingival swelling (Figures 3 and 4). The Cresco bridge was easily removed at review, the overgrowth excised and bridge adjusted for easier hygiene.
A patient with oral dystonia was restored with a cement retained restoration but with additional Bredent screw fixation (Figures 1 and 2) providing a secure bridge, but easily removable for prosthetic maintenance if required.

A bridge was provided for a wind instrument player with the Isus system (Figure 5) allowing easy access should screw loosening occur.
The final case demonstrates the Cara system that has allowed a screw-retained bridge (Figure 6) to be provided in a case with facially inclined implants.



