 Peter Rabin reports back on Oral-B’s evening seminars with lectures by Professor Nicola West and Dr Phil Ower.
Peter Rabin reports back on Oral-B’s evening seminars with lectures by Professor Nicola West and Dr Phil Ower.
Oral-B continues its popular series of educational evening seminars with lectures by Professor Nicola West and Dr Phil Ower, covering the topics of erosion and recession respectively. On Thursday 3 November I attended the first of seven events taking place around the UK. The venue was the Hilton Hotel in Watford.
Nicola West

Professor Nicola West enlightened the audience with her presentation entitled ‘Clinical strategies to prevent and manage erosion’ in which she stressed the need for early identification of tooth wear. The BEWE (Basic Erosive Wear Examination) was the crux of the lecture – 0 signifies no erosion or tooth wear; one – there is initial surface texture loss, needing preventive care; two – there is distinct loss but under 50% of surface area (eg cupping of molars); three – there is more than 50% surface area loss (eg decrease in tooth crown height and proud restorations).
Risk factors include erosive foods, such as lemon, salad dressings, citrus fruits, grapes and roasted peppers, acidic soft drinks, hydrochloric acid (heartburn), toothbrushing on an erosive softened surface. Life expectancy is increasing, so tooth wear and hypersensitivity with opened tubules will increase. Statistics show that we must wait two hours after having a grapefruit, before toothbrushing, but fluoride, milk and cheese will help negate the acidity. The key risk factors are the frequency of the consumption of the erosive acid-containing beverages, the duration of the erosive acid exposure, high consumption of acidic fruit and vegetables, drinking alcohol – red and white wine are of similar acidity, the manner of drinking, eg sipping, finally, drinking acid drinks at night when the saliva flow is low. These habits have to be modified to reduce erosive wear.
Biological factors that can influence the rate and extent of erosion are the saliva flow and the fact that the acquired pellicle protects the enamel – however, a strong acid challenge will remove the pellicle.
As far as the risk assessment is concerned, we must ask the patient if he/she is aware of tooth wear, do a BEWE score and check the diet, look at the frequency of consumption and check if the patient is a lactovegetarian, checking the teeth for tooth wear may highlight gastric problems (for example dyspepsia) and finding out about the patients lifestyle may indicate risk factors such as sports drinks or acidic medications. Treatments are topical fluoride – stannous fluoride is advisable, tooth brushing but not after acid drinks and bonding methods only if absolutely necessary. Patients with BEWE three readings should be referred to a specialist.
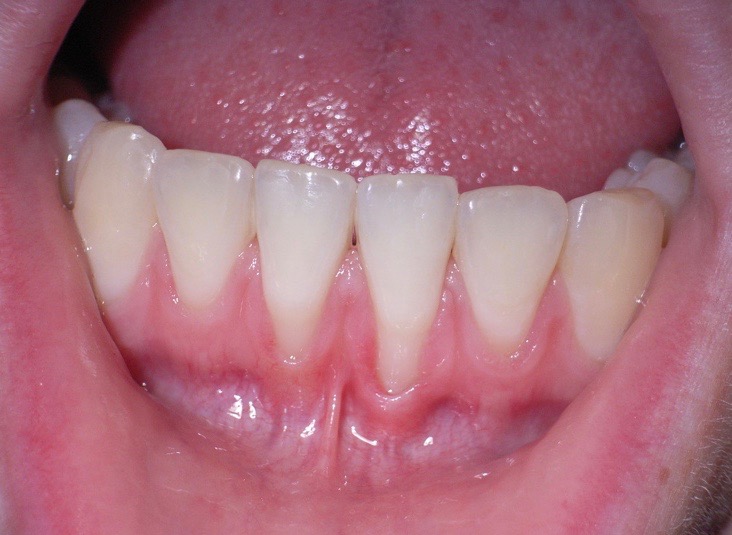
Following the ‘Lady Mayor’s Show’ would be difficult but Phil Ower presented ‘The recession obsession’ admirably. He stressed that recession is not a disease, it occurs naturally with age and is also part of the healing process when the patient suffers from periodontitis.
Phil Ower

It is important to realise that interdental recession is due to gingival disease; anatomical recession is natural or induced (mostly buccally) and there is no loss of the interdental papillae. Phil then described Miller’s classification of recession. Class one – the recession does not extend to the mucogingival junction and there is no interdental loss of attachment. Class two – the recession extends to the mucogingival junction but there is no interdental loss of attachment. Class three – the recession extends to the mucogingival junction and there is interdental loss of attachment but it is coronal to the recession defect. Class four – the recession extends to the mucogingival junction and there is interdental loss of attachment apical to the recession defect. Class one and two are mostly due to anatomy, whilst class three and four are mostly due to pathology. In the case of pathological recession, gingival shrinkage should be thought of as beneficial since post-therapy it is estimated that 75% of the healing process is due to recession.
The patient must be warned that the gingivae will shrink as a result of successful periodontal treatment. Phil stressed: ‘It is better to have a longer tooth than a tooth no longer’ and in addition ‘if you have periodontitis, recession is good for you’. The downside of recession is root caries, sensitivity and the unaesthetic ‘black triangle problem’. Grafts are not the answer in such cases. Composites can be used to fill in these areas or removable flexible gingival veneers may be considered, made in silicone from a special tray impression. These veneers cover the gingivae on the buccal surfaces and are highly retentive, having multiple paths of insertion.
Predisposing factors for anatomical recession are bone deficiencies – dehiscence and fenestration – and the gingival biotype. The causative factors are physical (toothbrushing, the opposing teeth, eating and oral jewellery), chemical (smoking) and biological (plaque-induced inflammation). Phil explained that frenal pull is a myth – the frenum rarely carries muscle fibres.
In the non-periodontal patient, reassurance regarding the recession is paramount. The toothbrushing technique has to be clarified; desensitisation can be carried out; root coverage with plastic surgery is another option but this is only suitable if there is no periodontal disease susceptibility. Surgical management is only for aesthetics and is not permanent.
‘Well fed’
Stephen Hancocks conducted the introductions and the questioning in his own inimitable style and the catering was copious and appetising, staying awake after a hard day in the surgery after being well fed, proved the success of the lecturers. Thanks to Oral-B who generously sponsored such an excellent evening.

