 Emma Hutchison describes the hygienists’ role in the rise of dental implants.
Emma Hutchison describes the hygienists’ role in the rise of dental implants.
When I qualified in 2001 I had sparse knowledge of dental implants and little experience in practice, very few people had dental implants at the time.
Now, increasingly more people are choosing to restore their dentition with implants to achieve a greater quality of life. This may be due to increased access to qualified and experienced implant-trained dentists and via referral to specialist clinics. Also, with the recent change in legislation for early pension release schemes and affordable payment options, financial barriers have been removed.
With the population living longer, the elderly are often choosing the implant route over dentures. Some patients >80 years are telling me that they do not need to spend their disposable income on things they used to, such as holidays and mortgages, so implants are a positive purchase for them. With this in mind, the dental professional has to consider factors such as medical problems, xerostomia, dexterity issues and the access to buying all the oral hygiene aids required to maintain implant health. Another consideration is to whom will ultimately be maintaining their oral care, will it be the patient or a carer?
My knowledge has been through colleagues, symposiums and dental literature, however in practice oral hygiene instruction has been dictated by my experience with different cases and patients. Oral hygiene aids need to be assessed for suitability for the patient and the restorative work done. Multi-unit and full arch fixed cases will have different needs to single unit implant cases, as will anteriorly placed units to posteriorly placed units. Challenges are to achieve the best possible aids to suit the implants and the patients and so an awareness of what is available, and adaptability is key to preventing implant failure.
What to recommend
Whenever possible I see the patient prior to implant placement to create a healthy ‘flora’ and establish a good oral hygiene regime. Any existing periodontal disease is treated prior to placement of the implant, and also after the restoration is placed for appropriate advice for implant maintenance.
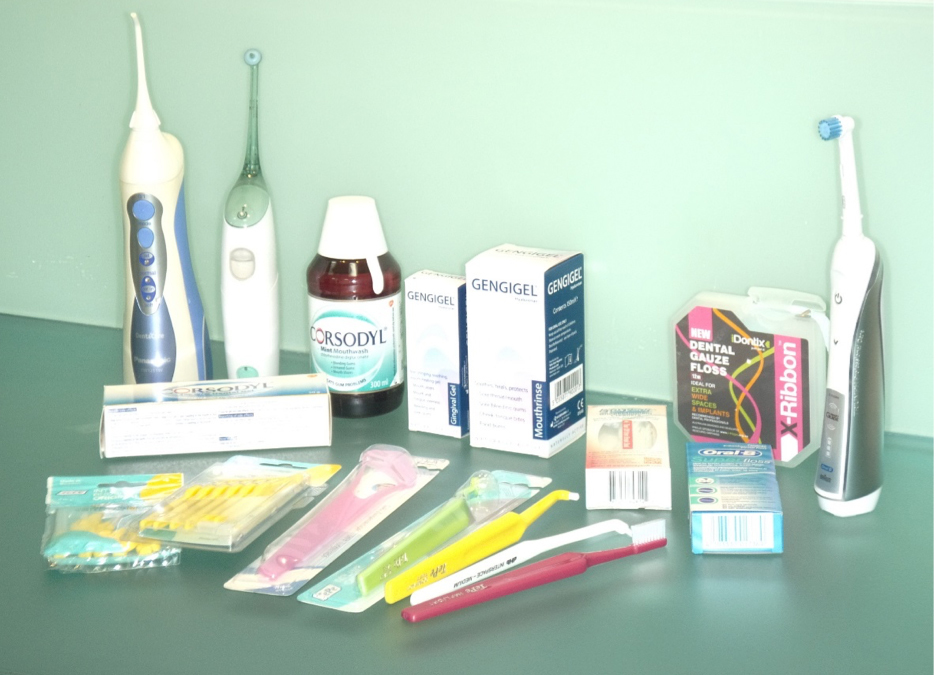
There are various oral hygiene aids available on the market and the aim is to remove the plaque and biofilm, which, if left, can lead to peri-implant mucositis, which is reversible, and peri-implantitis, which can ultimately lead to implant failure. A variety of choices (Figure 1) can include:
- Manual toothbrushes, including implant specifically designed and with bendable necks
- Electric toothbrushes, oscillating, side to side and sonic types
- Single tufted and angled implant designed
- Home irrigation (water flossers), units and portable type
- Air flossers
- General floss in various thickness
- Super floss in various thickness, with and without threaders
- Tongue cleaners, some electric toothbrushes have this mode now
- Chemical and non-chemical adjuncts such as chlorhexidine gluconate and hyaluronan.
Implant maintenance
If it is a single unit or an easily accessed restoration I prefer to recommend a thicker super floss without a threader, which can be curled under the crown to contact the implant itself. If there is existing inflammation I would advise using chlorhexidine gluconate, which is bactericidal, until it resolves and thereafter the hyaluronan in a gel, which encourages healing by the proliferation of fibroblasts, can be used long term.
In multi-unit bridges and difficult accessed restorations, the water flosser, if used correctly, can be very effective, especially in less dextrous patients as they are usually quite bulky. In general all of the above listed products I will recommend depending on the case and patient, especially tongue cleaning to keep the flora healthy.
Interdental brushes should be assessed at each visit to check if the size used is suitable to contact the implants, an adjunct can also be recommended with these. If there are dexterity issues you could advise foam pipe lagging from hardware shops, which come in different diameter holes of which the toothbrush can be slotted into.
Crown and bridge dental putty can be used to adapt and aid in surgery (but this can be expensive for the clinic), there is also a product available on Amazon called ‘SUGRU’, which is similar and self-cures in two days for smaller aids such as interdental brushes etc.
Implant design
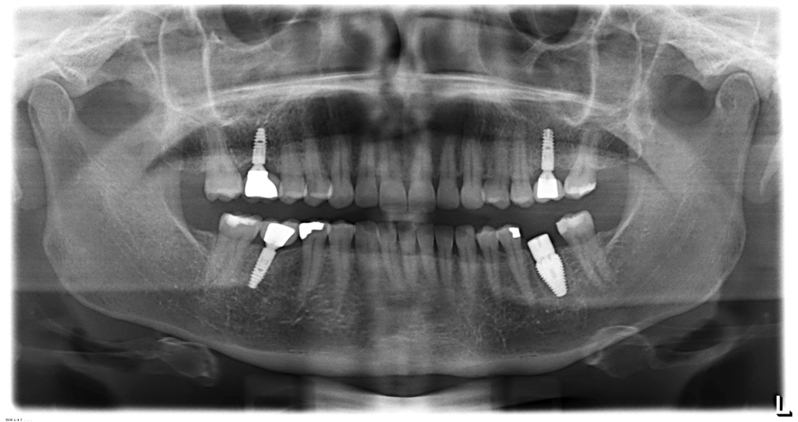
Over the years different designs for implants have been developed and the long-term success of implants can be determined by its design. Some implant designs coat the entire length of the implant, which is thought to encourage better osseointegration, however, this can be problematic if the bacterial complex attaches to the roughened implant surface with consequential peri-implant disease. However, if the design of the implant has a smooth polished collar at the soft tissue end then bacteria cannot hide in the roughened surface or within the screws and so it is more self-cleansing.
The design for the prosthetic restoration also needs to be considered so it avoids overhangs and areas that can foster bacterial growth. A ‘lollipop’ effect, which is ultimately more difficult for the patient to keep clean, should be avoided whenever possible (Figure 2). This theory concurs with an article in Dentistry magazine, (May 2017), which discussed a recent study looking at ‘Microthreaded implants and crestal bone loss: a systematic review’.
It is also worth considering that in the present world of potential litigation, especially with implants, it is essential to have correctly written notes. The health of the implant should be noted including signs of peri-mucositis or peri-implantitis and bleeding on probing, mobility and any oral hygiene advice given. If the dental software allows, then pre-written notes can help to achieve this for convenience and edited to add extra information. Studies show that a three-monthly visit maintenance plan should be recommended so any problems can be picked up and addressed quickly. An example that I use after my general patient notes is below.
‘The patient was advised about peri-implant mucositis and peri-implantitis risks associated with noncompliance of the oral hygiene advice given. Advice for three-monthly implant maintenance recall visits were advised.’
In conclusion, every restoration, systemic and oral health, age and dexterity will mean possible different approaches to achieve implant maintenance and there may be other aids and devices on the market that work well for different patients. There is no one rule that works for all, so the challenge is knowing when to recommend one over another, and to be adaptable!


