Olumide Ojo describes how short-term orthodontics, bleaching and bonding restored function and aesthetics.
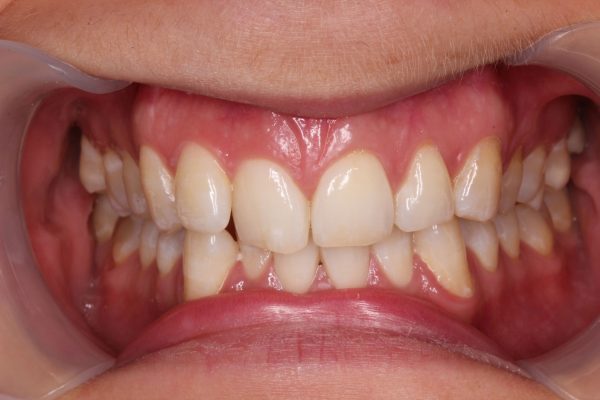
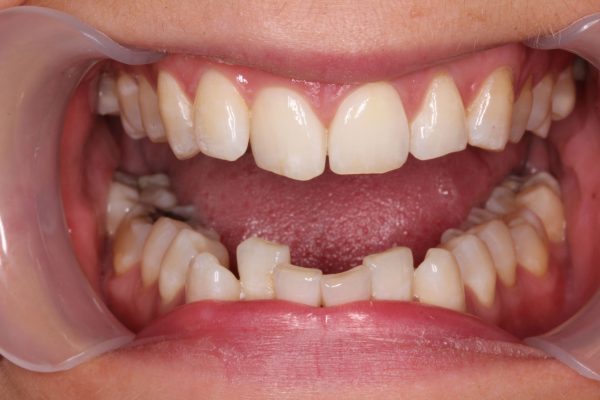
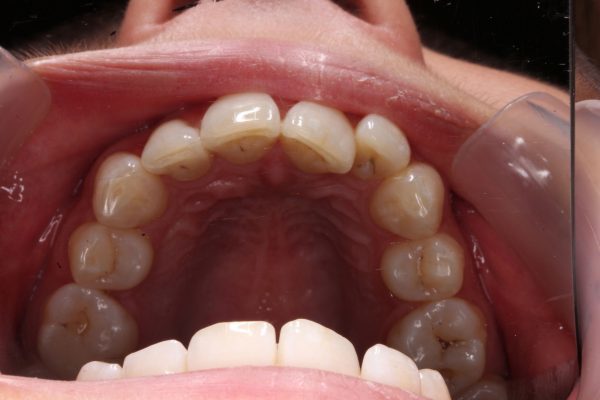
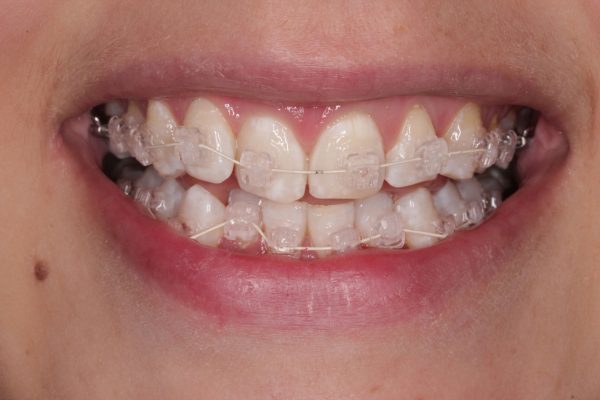
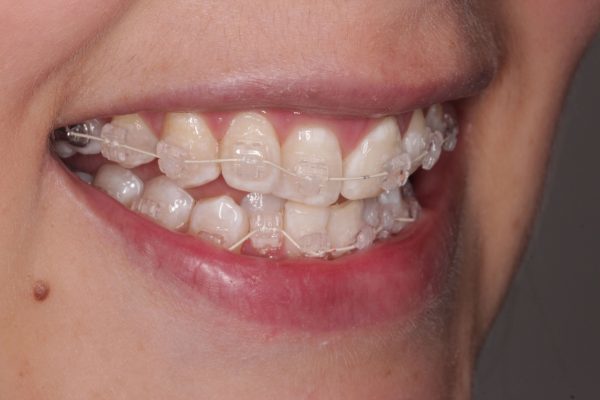
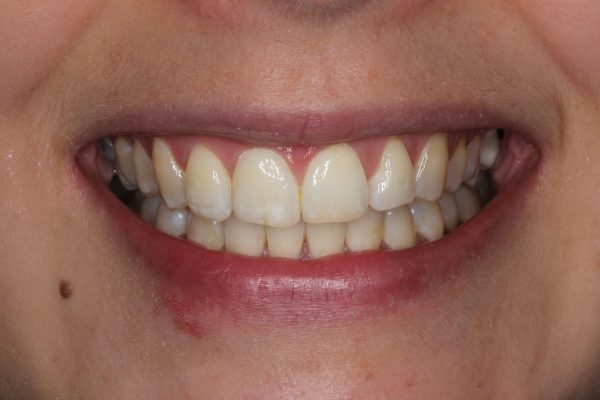
A 24-year-old female patient came to see me because she was concerned with her crowded upper and lower front teeth (Figure 1). She was very unhappy with her smile and general tooth colour (Figures 2 and 3) and wanted them re-aligned and whitened.
The patient had undergone orthodontic treatment in her mid-teens and reported that she was advised she need not wear her retainers beyond a year post-treatment. She felt that her teeth had gradually been moving back and wanted to rectify this.
She was preparing to be a chief bridesmaid at her best friend’s wedding and was self-conscious of her smile. The prospect of her teeth being on display at such a major event had prompted her to seek immediate treatment.
Initial assessment
A full dental examination was undertaken to assess her existing dentition and to ensure that she was a suitable candidate for elective aesthetic treatment. An orthopantomogram (OPG) X-ray was taken to assess all root morphology, potential root resorption and wisdom teeth. No significant root resorption was noted.
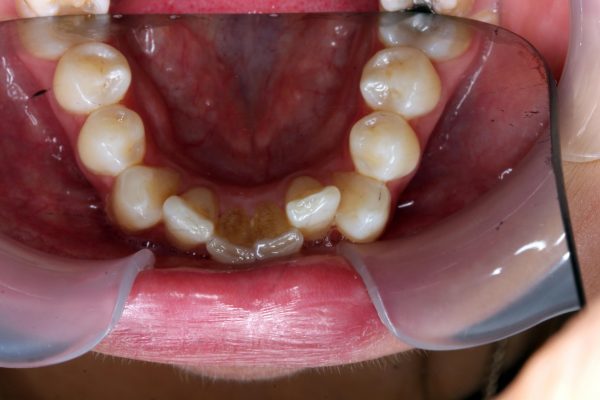
A full dental and orthodontic summary was completed. The patient had a class I skeletal and incisor relationship and half unit class II on molars left and right (Figure 4). There was crowding of 3mm on the upper and 5mm on the lower anterior sextant. No posterior crowding was found. A diagnosis of orthodontic relapse and late lower arch crowding was made (Figure 5).
A functional assessment revealed a moderate bruxist habit with attrition. Exposed dentine was apparent, and mild attrition had resulted in incisal edge wear of the upper and lower incisors. The loss of smooth canine guidance had led to group function that was likely to increase the anterior wear further.
Treatment plan
The treatment plan aimed to significantly improve the upper and lower anterior crowding, whilst levelling and aligning the incisal edges and gingival margins. The teeth would be whitened to improve general colour, before the worn upper incisal edges were restored with composite resin.
Finally, the upper and lower anterior teeth would be retained indefinitely, whilst maintaining the existing dental midlines and posterior occlusion. A variety of different fixed and removable orthodontic appliances were discussed in detail, including referral to our in-house orthodontic specialists.
The patient requested clear, aesthetic fixed appliances, rather than removable aligners, due to better compliance and speed (Figure 6). She had a very tight deadline of seven months until her friend’s wedding. On the basis that she was happy with the position of her posterior teeth and only required anterior alignment, she chose Cfast cosmetic alignment.
I use Cfast anterior alignment appliances for my fixed orthodontic cases. This is a system of accurately pre-positioned, clear, ceramic brackets set up by an orthodontic laboratory technician. The brackets are then transferred into carrier trays ready to be bonded intraorally. They are placed in the best possible position under optimum conditions outside of the mouth. This saves significant time and helps reduce operator error during the bonding process.
Two impressions were taken using Kulzer Xantasil. Relevant radiographic and photographic views were obtained for full assessment and planning of the case. Xantasil has become my material of choice for orthodontic and diagnostic impressions. I like the stability of the material and that multiple models can be poured from just one impression.
The case was discussed with Triple O Dental Laboratory in Birmingham. It was accepted as suitable for anterior aesthetic alignment with Cfast, with a prescription of an estimated interproximal reduction (IPR) of 3mm spread over the duration of the treatment.
Orthodontics
The pre-positioned bracket trays were carefully checked on the models and also tried in the mouth to ensure a passive fit. The teeth were isolated and the brackets attached following standard resin cementation protocols.
A latex-free lip and cheek retractor was used to aid cementation, help improve moisture control and to provide a greater visual field. A series of 0.014 round nickel titanium wires were engaged into the self-ligating brackets (Figure 7). The brackets have a discreet gate system, which are opened using a special tool or a small ended straight probe. The gates are then simply shut, once the wire is ligated, using a finger or flat end of tweezers.
IPR was not carried out at this stage to allow arch development and rounding. This helps the most crowded contacts to align and be more accessible for IPR when needed. Postoperative and oral hygiene instructions were reinforced to the patient.
The patient attended for review at four weekly intervals. The properties of the nickel titanium wire allowed it to be rounded to aid the slight proclination of the teeth. This helped to gain significant space required for alignment. From the second month, IPR was carried out selectively on the necessary contacts, with the most easily accessible contacts opened first.
The nickel titanium wires were changed from 0.016 to 0.018 as the arch aligned. The repositioning of a few brackets and the use of quick-tie ligatures were required to express full movement. The orthodontic treatment was completed with a continuous power chain to gather up and close any residual spacing (Figure 8).
Debonding and bleaching
Alignment was completed and the patient approved the end result. Temporary freehand fixed retainers were placed and bonded using Ortho Flex wire and Kulzer Venus Bulk Fill, before removing the nickel titanium wire or brackets. This would prevent any inadvertent relapse due to vertical pressure, potentially causing the teeth to move.
The brackets were then debonded using a selection of composite removal burs (Figure 9), ensuring that no residue was left on the teeth that could affect the whitening stage. Impressions for Essix retainers and whitening trays were taken with Xantasil and sent to the laboratory.
The Essix retainers and whitening trays were fitted and checked. Tooth whitening was undertaken for a period of two weeks using 16% carbamide peroxide overnight (Figures 10 and 11). Once complete and the patient was satisfied with her tooth colour, a further two weeks was allowed for optimum bonding to occur.
Composite restoration and finishing
The patient returned for restoration of the severely worn incisal edges with direct composite bonding (Figures 12 and 13). Each tooth was restored using Kulzer Venus Pearl. I like Venus Pearl because of its strength in thin sections. It also has a wide range of shades that are equally good used as a mono shade, or as part of a layering technique. Venus Pearl also has great polishing qualities.
In this situation, I personally use a composite heater to allow softer handling. A working shade was selected using small portions cured on the teeth before isolation, to ensure no dehydration took place. The fixed retainers were removed before treatment commenced.
A diagnostic wax-up and stent were used to construct a palatal matrix shelf using translucent Clear Light (CL)shade. The facial layers were created with high chroma Opaque Light Chromatic (OLC) dentine shade, followed by the enamel Bleach Light (BL) shade and finally the CL shade (Figures 14-16). The teeth were built up using a freehand composite technique.
High predictable polish
The composite restorations were polished using a full range of Sof-Lex discs and the Kulzer Venus Supra polishing burs and paste. I use Venus Supra because it is a simple, efficient system, which achieves a high, predictable polish, with good results every time. The occlusion was checked and refined in all excursions. I was able to restore the occlusion to allow good anterior disclusion and canine guidance on lateral excursions.
Final impressions were taken using Xantasil for post treatment digital models, and new fixed and Essix retainers. Archiving the digital study images reduces my reliance on storing the stone models.
At her last review appointment, all before and after photographs were shown to the patient. Final occlusal analysis and polishing was completed at this stage. The orthodontics took less than five months and the whole case was completed in six months (Figures 17 and 18). The patient was delighted with the final result (Figures 19 and 20). All treatment was finished five weeks before her chief bridesmaid duties commenced.
No two alignment, bleaching, and edge bonding cases are the same. Each highlight new learning objectives. Although this case went according to plan, I spent a long time at the consent stage managing the patient’s expectations of the treatment. We discussed the limitations of anterior aesthetic alignment and of composite bonding.
In my view, it is important that we do not overpromise what can be achieved. When a case is too complicated or if we are unable to meet a patient’s expectations, I would advise referral to specialist colleagues or more experienced clinicians.