 Matt Everatt and David Bretton examine clinical literature on tooth whitening trays
Matt Everatt and David Bretton examine clinical literature on tooth whitening trays
Tooth whitening is very common practice in dentistry today, made famous by celebrities in the 1980s, and was initially thought to have been discovered by accident by a group of dentists using peroxide to treat gum disease (Kurthy, 2016).
The UK tooth whitening industry is believed to be worth over £40 million, as more consumers seek the white, healthy smiles endorsed by many celebrities, according to the 2018 National Smile Month campaign. Market research shows that 99.2% of us believe our smiles are an important social benefit, according to research firm Hexa Research, whilst a further study, published online, found that 48% of adults believe a person’s smile is the most memorable feature upon first meeting.
Haywood (2003) suggests that the efficacy of whitening is greatly improved when the hydrogen peroxide level is around 6%, and custom-made dental trays are used to hold the gel close to the teeth for a period of around two hours. Carey (2014) also supports this approach, concluding that hydrogen peroxide and carbamide peroxide tooth whitening is safe and effective. He felt that ‘home based bleaching (following manufacturer’s instructions) results in less tooth sensitivity than in-office bleaching.’
Cosmetic dentist, Zase (2009), lists sensitivity and compliance as the two main problems associated with tooth whitening. The whitening procedure could help reduce sensitivity, whereas tray design can directly help improve compliance. It is therefore important to consider the design and use of custom-made bleaching trays to achieve the optimal results in a timely and safe manner.
Bleaching tray design
Bleaching tray designs have been debated amongst dental professionals over the years, with many opinions formed on the basis of very little scientific evidence to support any particular design. Many assumptions are made and logic used in the absence of science when discussing the specifics of tray design.
There are several technical specifications used, such as: scalloped margins, straight cut margins, extension beyond the gingiva, and reservoirs. The process of thermoforming is also debated; Mizuhashi and Koide (2017) found that vacuum-formed appliances maintained material thickness, whilst pressure formed appliances obtained a better fit.
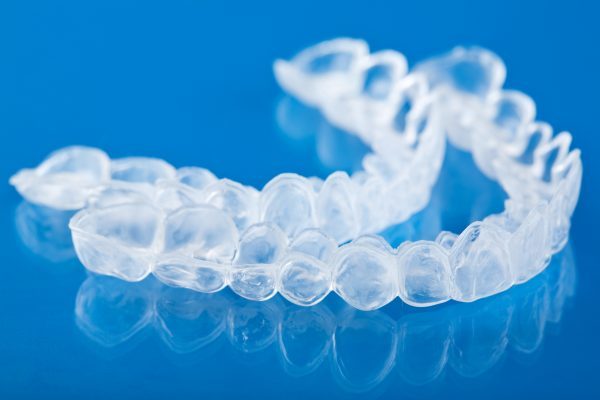
Model thickness can also affect the fit of the finished tray. Due to the morphology of the oral tissues and dentition, it is difficult to provide a standardised model size in which to form the tray. Therefore, material thickness can vary from model to model. Mizuhashi and Koide (2017) also noted that the marginal fit of the pressure formed appliances was significantly improved by pressure forming appliances.
Reservoirs or no reservoirs?
Matis et al (2002) showed that there was little difference in results in terms of shade difference when comparing trays with and without reservoirs. Despite there being minor shade differences when using a colourimeter, the shade difference was below the threshold of visual differentiation.
It would appear that the importance of using reservoirs is linked to how well the margins are sealed. Trays that are scalloped are inevitably more flexible and will allow more bleach to escape the tray, therefore requiring a larger amount of bleach present in a reservoir.
There are clinicians, such as Kurthy (2016), who advocate the use of a reservoirs and finishing the tray exactly at the gingival margin. The margin for error from the impression stage to the dental laboratory finishing the trays is high.
Further anecdotal evidence suggests that the hand trimming and finishing process deforms the thermoformed tray, leading to a tray that is not as well sealed at the peripheral margins.
Haywood (2008) also states: ‘Reservoirs are not needed to bleach; they merely reduce the tightness of the tray. Teeth bleach just as quickly without the reservoir as they do with.’
Dosing dots
A relatively new method introduced in the tray design are ‘dosing dots’ or ‘dimples’. Not to be confused with reservoirs, these small areas in the trays are designed to help the patient add the correct amount of gel to each tooth and not overload the tray.
Overloading the tray can lead to sensitivity, non-compliance, and gingival irritation (Zase, 2009). Dosing dots are therefore recommended to reduce the risk of complications associated with home tooth whitening.
Gingival contouring or straight extension?
Theory may suggest that gingival contouring or scalloping could reduce the amount of bleach having mucosal contact; however, there appears to be no cited references to the benefits to scalloping trays. One could argue that by closely following the gingival margin with a scalloped designed tray, the surface area covered is less and therefore leads to less mucosal irritation, although this theory is not supported by any literature.
To the contrary, Curtis et al (1996) demonstrated in a group of 52 patients that there was no soft tissue damage in any of the sample group as a result of the bleaching regime. To further support that the extension of the bleaching tray beyond the gingival margin has no effect on efficacy or sensitivity, Morgan et al (2015) demonstrated in their group of 20 subjects that there was no statistical difference in how effective the bleaching was, nor did the extended or non-extended trays cause any more or any less sensitivity.
There appears to be a lack of clinical evidence to support gingival contouring. Scalloping is only needed with higher concentrations of peroxide. According to Haywood (2008), considering the 2013 laws in the UK that restricted the use of higher concentration ‘in office’ bleaching, the need for scalloped trays is no longer an issue in terms of gingival contact.
Research by Cowley et al (2012) compares the fit and retention of thermoplastic retainers in the different design of finishing, these being: scalloped, straight cut at the gingival zenith, and a straight cut 2mm beyond gingival zenith. The best retention was found in the appliances finished 2mm beyond gingival margins, with those finished at the gingival margin the poorest.
Although the materials cannot be compared like for like, finishing with a straight-line cut will increase the stability of any thermoformed appliance. This means that the bleach will likely remain in contact with the tooth surface longer, possibly increasing the efficacy of the bleaching material.
To further support the benefits of cutting the trays straight in a line 2mm above the gingival margin, Cowley et al (2012) also suggests that the appliances should ‘be more comfortable than before, because there will be less risk of them impinging on the unattached marginal gingiva’.
With the current literature stating that there is no benefit in using reservoirs, it would appear counter-effective to have gingivally trimmed trays. Trays with a straight cut margin of approximately 2mm beyond the margin will give better stability (Cowley et al, 2012). The additional flexibility that comes with scalloping a tray can also be problematic in bruxism patients, as the tray is more prone to bending and emitting bleach in comparison to straight cut trays.
Tray material
There are several materials that are commonly used for bleaching trays, with 1 or 1.5mm soft ethylene-vinyl acetate (EVA) being the most common. In recent years, there has been an introduction of material designed for use in bleaching. A foam-lined tray, for instance, was introduced, with the notion that the foam would have an advantage in holding the bleach over standard trays. However, Haywood et al (1993) proved there was no difference in the clinical results.
Manufacturers have introduced a material that has a firmer feel to standard EVA material, commercially available as a ‘bleach tray material’, with the majority of the manufacturers offering 1.5mm semi-rigid as the most popular type for bleaching.
Conclusion
In conclusion, this review has highlighted that there is only a limited number of clinical studies available discussing tooth bleaching. Furthermore, there are even fewer studies to support bleaching tray designs in relation to their effect on treatment. Further studies should consider tray designs in relation to compliance alongside the efficacy of the whitening gels.
With the limited clinical evidence, a conclusion can be drawn that a bleaching tray should have some specific design features, whilst other features appear to be operator-led, without having any proven clinical benefit other than it being accepted by the clinician and patient as acceptable.
There is no evidence to show that reservoirs improve shade reductions, and there is little evidence to support their use other than in trays that are trimmed gingivally to aid the seal. Scalloping would also appear to be counterproductive in terms of patient comfort and tray stability.
An optimal tray design should have a good peripheral seal around the gingival margin, be trimmed straight just beyond the gingival margin to improve seal and stability, and provide comfort and, therefore, increased compliance for the patient.
Although there is no published data to support ‘dosing dots’ or ‘dimples’ on the labial surfaces, it appears to be a useful tool in demonstrating to patients how much bleach to administer per tooth.
References
Carey CM (2014) Tooth whitening: what we now know. J Evid Based Dent Pract 14(Suppl 1): 70-76
Cowley DP, Mah J, O’Toole, B (2012) Effect of gingival margin design on retention of thermoformed orthodontic aligners. J Clin Orthod 46(11): 697-702
Curtis JW, Dickinson GL, Downey MC, Russell CM, Haywood VB, Myers ML, Johnson MH (1996) Assessing the effects of 10 percent carbamide peroxide on oral soft tissues. J Am Dent Assoc 127(8): 1218-1232
Haywood VB, Leonard RH Jr, Nelson CF (1993) Efficacy of foam liner in 10% carbamide peroxide bleaching technique. Quintessence Int 24(9): 663-666
Haywood VB (2003) Frequently asked questions about bleaching. Compend Contin Educ Dent 24(4a): 324-338
Haywood VB (2008) The ‘bottom line’ on bleaching 2008. Inside Dent 4(2): 2-5
Kurthy R (2016) The myth of bleaching lights and lasers
Matis BA, Hamdan YS, Cochran MA, EckertGJ (2002) A clinical evaluation of a bleaching agent used with and without reservoirs. Oper Dent 27(1): 5-11
Mizuhashi F, Koide K (2017) Formation of vacuum- formed and pressure-formed mouthguards. Dent Traumatol 33(4): 295-299
Morgan S, Jum’ah CC, Brunton P (2015) Assessment of efficacy and post-bleaching sensitivity of home bleaching using 10% carbamide peroxide in extended and non-extended bleaching trays. Br Dent J 218(10): 579-582
Zase M (2009) Bleaching: preventing common problems. Dent Today 28(3): 120-121

