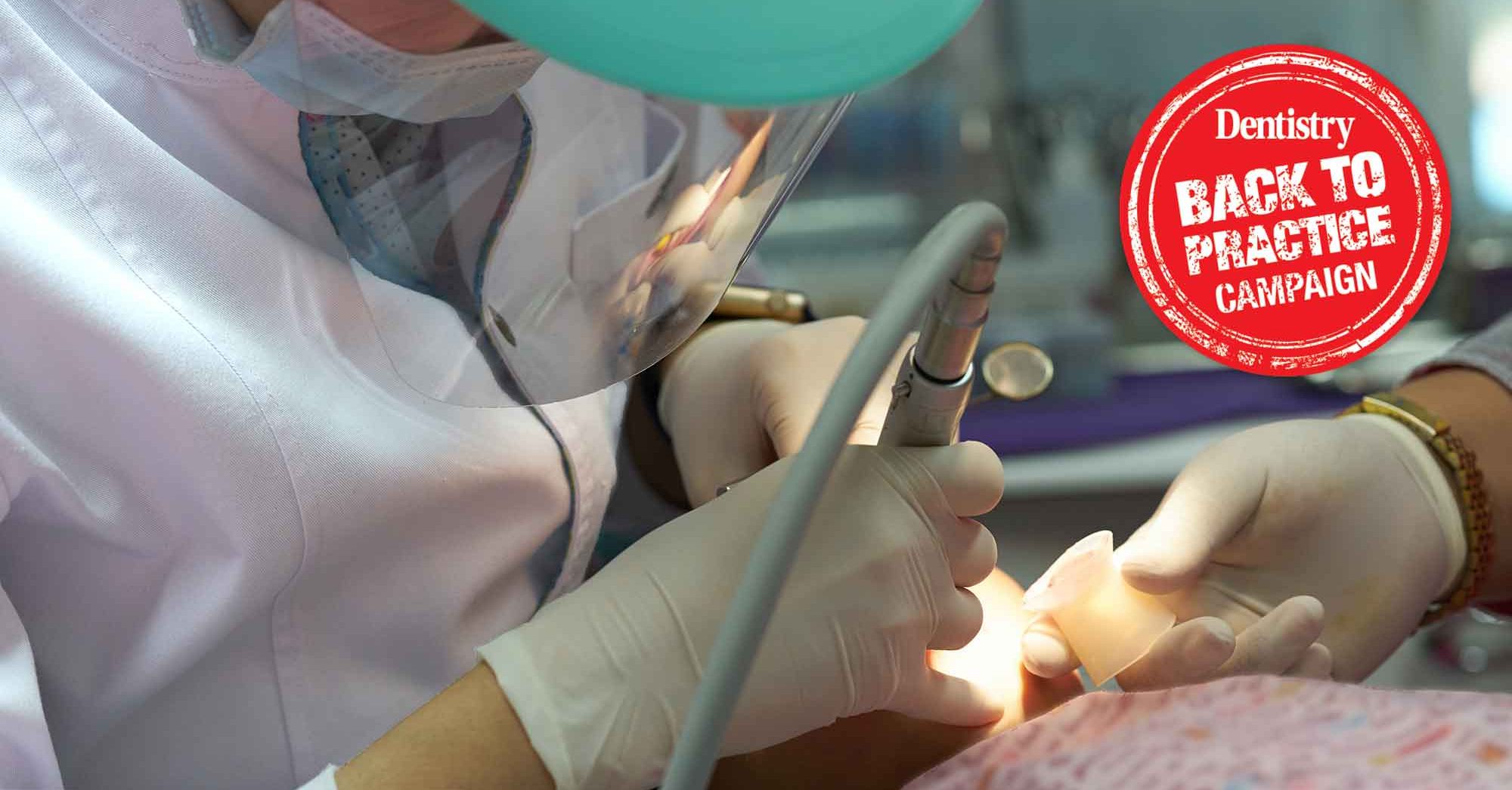
 As dental practices start looking at what they might need to reopen once the COVID-19 lockdown ends, Seb Evans explores what the cost of this might be.
As dental practices start looking at what they might need to reopen once the COVID-19 lockdown ends, Seb Evans explores what the cost of this might be.
Boris Johnson recently announced the first stage of ending the current lockdown. Despite Sara Hurley, CDO for England, saying dental guidance remains unchanged, many practices are now looking at what they may need to do when the time does come to reopen.
There is currently no official guidance for dental practices to follow once they do open. However, there is some consensus from associations around the profession what dentistry may look like.
Here we decide to look at what a post COVID-19 dental surgery might look like. Including the financial costs of coming back to work. For the most part we use NHS England’s standard operating procedures (SOP) for urgent dental centres. We’re assuming the same applies for private practices.
Face masks
Cost range estimate – £5-£200
NHS England’s SOP says FFP3 face masks are required for all aerosol generating procedures (AGPs). The HSE has since stated that FFP2 and N95 respirators (filtering at least 94% and 95% of airborne particles retrospectively) may be used if FF93 respirators are not available. The price of the face mask can vary. It depends on whether you are purchasing a single-use mask or a reusable mask with replaceable filters.
The price of FFP3 face masks will vary widely compared to what it was before the coronavirus outbreak.
A quick search online suggests, due to the shortage of FFP3 face masks, a single FFP3 mask could start at around £5 (if you can get hold of them). Along with this, clinical staff will need to wear visors or disposable eye protection. These protect the eyes of the wearer and can cost as little as a couple of pounds each.
A powered air respirator that protects the eyes and comes with a breathing filter attached may reach over £200.
‘A lot of practices are rushing out to get PPE, fit testing etc,’ Alfonso Rao, principal dentist at Queen Square Dental Clinic, says. ‘But all without full guidance yet.
‘There are a lot of buying groups that are getting PPE from various sources. Some of those are not fit for purpose. There are a lot of new groups working together to come up with suggested SOP. That hopefully will bring some clarity.
‘A survey conducted amongst 4,292 dental professionals shows only 7% experienced COVID-19 symptoms prior to the lockdown. This is much lower than the general population, and can we cnan attribute this to their use of PPE.
‘FFP3 masks also need to fit testing to be effective. It’s not always easy to get the same masks. There is really little extra protection that FFP3 mask offers compared with FFP2 (protection 0.4%).
‘Furthermore, for non-AGPs, there is no evidence that respirator masks add value over standard fluid resistant masks when both are used with recommended wider PPE measures.
‘It makes practical sense based on this evidence to use standard surgical masks for non-AGP and if the other protocols are employed, fit checked FFP2 masks for AGP procedures.
‘A lot of practices that are already in financial difficulties after this crisis. They are considering options to absorb these increased costs.’
Disposable gloves
Cost range – double
Not all staff will need to wear all types of PPE. For instance, reception staff may be exempt from wearing disposable gloves. But it is recommended that they wear a standard surgical facemask.
The donning policy between areas also varies slightly. For example, some London hospitals are currently advocating the use of two pairs of disposable gloves. Both above and below the cuffs of fluid resistant gowns. The operating procedure of the local area will to some degree govern overall costs in this regard.
Disposable gowns
Cost range – from 10p to £15 per patient
According to NHS England, clinicians should wear disposable plastic aprons for non AGPs. For treatments involving AGPs, clinicians should wear fluid-resistant gowns. However, if dental teams use non-fluid-resistant gowns, they must wear a disposable plastic apron underneath.
A quick search online suggests practices can purchase plastic aprons for around 10-20p per apron. Whilst the gowns are a little pricier at around £3-£4 in normal times but increasingly reports show that many go for far more.
Some companies are looking at reusable options that can be laundered. These have a higher initial outlay but reduced future costs.

Suction systems
Cost range – £2,500+
Currently the NHS says dentists should not carry out any aerosol generating procedures unless within a UDC with enhanced PPE. This will probably remain the case for the foreseeable future. However, certain activities such as preparing teeth, removing fillings, crowns and bridges all produce aerosols.
Some intraoral suction systems can offer performances of around 300l/min, which dramatically reduces the risk of infection for everybody in the surgery.
Suction systems might cost practices around £2,500 for an effective system. And a wide-angle cannula would cost about £15 for a set of four.
Before purchasing a new system, a test by a qualified engineer to ascertain the suction volume of their existing unit might cost around £100.
The use of rubber dam and high-volume suction significantly reduces the potential for contaminated aerosol too.
We await to see other solutions to reduce aerosols post COVID-19.
Reception screens
Cost range – around £50+ depending on the size of reception
Clear screens on reception desks will help shield and protect staff from viruses that patients might bring in. Prices for these screens can vary substantially depending on the size of the reception desk and the materials used.
A quick search online suggests a sneeze guard might be available for as little as £50, but could possibly reach thousands depending on the size of the reception and style of the screen the practice would like.
Dentist Neel Kothari told Dentistry Online: ‘It’s incredibly hard to judge how effective these measures are likely to be. I myself have invested in counter protectors largely to reassure my reception staff and demonstrate to patients that we are taking their health and safety seriously’.
Air purifiers
Cost range – zero
The BAPD’s Return to practice position paper suggests air purifiers don’t offer any further protection against COVID-19.
The NHS also hasn’t published any recommendations on air purifiers to help control the spread of COVID-19.
Studies have linked coronavirus transmission to air-conditioning units. However, there is no consensus at the moment to confirm whether air-conditioning units do actually help with transmission.
Dr Kothari said: ‘There are a few glaringly obvious issues with air purifiers. Firstly, we as clinicians will always be between the patient and the unit. Secondly, there is a distinct lack of evidence demonstrating effectiveness and finally, if needed, what standard do we require? Could we end up spending a lot of money only to be told they need to be upgraded?
‘However, to many dentists the costs of the units are a relatively inexpensive way to demonstrate to their patients that they are doing everything they can to ensure safety.’ At this moment Neel Kothari says he is keeping his options open and may reconsider if there is further evidence to support their use.
Patient numbers
Cost range – halved
Assuming patients are happy to return to the practice the day it reopens, there are other matters to consider.
To maintain social distancing between everybody in the building will mean a maximum number of patients can enter the practice at any one time. The surgeries would also need extensive cleaning between each appointment, taking up more time.
Some have suggested practices will only be able to work at 50% capacity due to the extra clean down and number of people allowed in the surgery at any one time.
This will cause income to reduce in the short term across dental practices and pose several challenges to practices dependant on hitting UDA targets, if these remain unchanged.
Conclusion
‘SARS-Cov-2 is a novel virus and for a small number of individuals lethal. The global impact has been swift and severe,’ Judith Husband, GDP and owner of a consultancy company in dentistry, concludes.
‘In the UK we are facing the second highest country mortality rate and traditional epidemiological approaches many other countries use, we abandoned in late March.
‘Testing and tracing is now a priority. But with a fragmented infrastructure and significant organisational challenges to overcome.
‘Dentistry sits within this landscape and our risk management needs to be cognisant and responsive to our local situation.
‘In early May the Cochrane Oral Health Group published a rapid review of country-based guidance – Recommendations for the re-opening of dental services: a rapid review of international sources. As a novel virus there is a minimal evidence base with many decisions currently focusing on the mitigation of risk and what is practicable.
‘The guidance published by 11 countries fails to reach a clear consensus and we await the publication of the UK standards document. It is essential we agree professional standards that cover the UK to support dental teams in our return to work and guide our future decision making.
‘Without an evidence base, and with little clear agreement globally, it is a unique time for dentistry but also an opportunity to reshape the delivery of our care.
‘Dental care is an essential service and needs to be available to patients throughout this pandemic, it will need to be flexible and sensitive to changes in community transmission and demand on PPE. The sector must be financially sustainable and this is perhaps the greatest challenge we face. A significant reduction in numbers of patients is likely, there may be future waves of disease necessitating a significant reduction in clinical care provision, increased demand on PPE globally will drive up costs and availability. The traditional models for NHS and private dental care provision must change.
‘The Minamata Treaty amalgam phase down, the climate emergency, together with changing demographics and prevalence of dental disease were already drivers for change prior to COVID-19. The virus is supercharging that need for change.
‘Community-based prevention working across health and social care, early clinical interventions with minimally invasive technologies must rapidly develop. We need to engage with patients differently with more targeted care utilising digital technologies for shielded and hard to reach groups.
‘Working longer hours and charging higher fees is not the solution. Structural change in the delivery of dental care, within the mixed economy is essential.’
This article only provides a hypothetical look at what dental practices might require if they were to open. It is not an extensive list and its intention is not to provide any suggestions for equipment. Nor is it a checklist for equipment practices will need to open.


