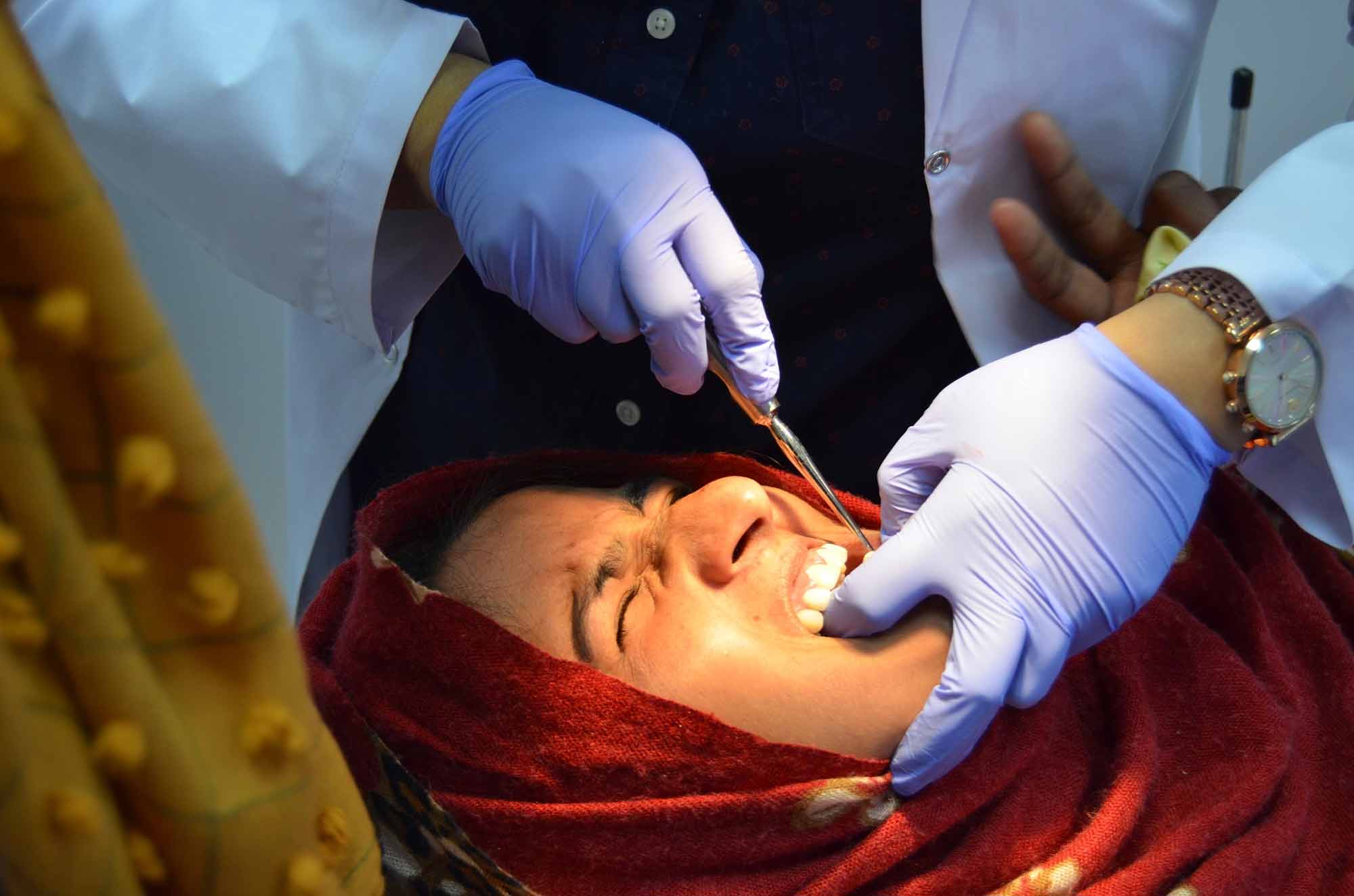
 Dr Thanaa Abdullah talks about her experience helping to create a dental department at a hospital in Kashmir.
Dr Thanaa Abdullah talks about her experience helping to create a dental department at a hospital in Kashmir.Since qualifying from dental school, I’ve always tried to give money to charity. This would usually be a monthly direct debit that I could set up and forget about.
I would give bigger lump sums when there was some disasters. I’d also give during times of war when donations were needed more. However, I never felt like I was doing enough.
Midland Doctors Charity was established after a devastating earthquake hit Kashmir followed by flooding of the region. A team of doctors from the midlands region travelled to Kashmir, setting up emergency camps to treat those effected by the disaster.
After seeing how poor and isolated the region was, they set out to build a much needed hospital in the area. Their vision was to use the NHS model and provide free treatment to those in need. The hospital currently has paediatrics, cardiology, pharmacy, pathology, general medicine, general surgery, urology and radiology departments.
Preventable deaths
The hospital on average receives approximately 200 patients per day with various complaints. The local population will suffer with pain and symptoms for months or years with no hope before the hospital was built.
A lot of preventable deaths occur because of poverty and the lack of services for medical care. These preventable deaths often leave behind widows and children whose lives deteriorate and they become helpless.
With plenty of room to develop further departments, and the knowledge that approximately 15-20 patients attending the hospital on a daily basis, I made the suggestion to set up a dental department. The trustees of the charity had no knowledge of dentistry although appreciated the need for emergency dental care.
I was given the green light to proceed providing I raise the funds and that dentistry didn’t become a drain on the central funds for the hospital. The principals of the hospital is to treat patients with compassion, ensure accountability is in place, treat patients with respect and provide education.
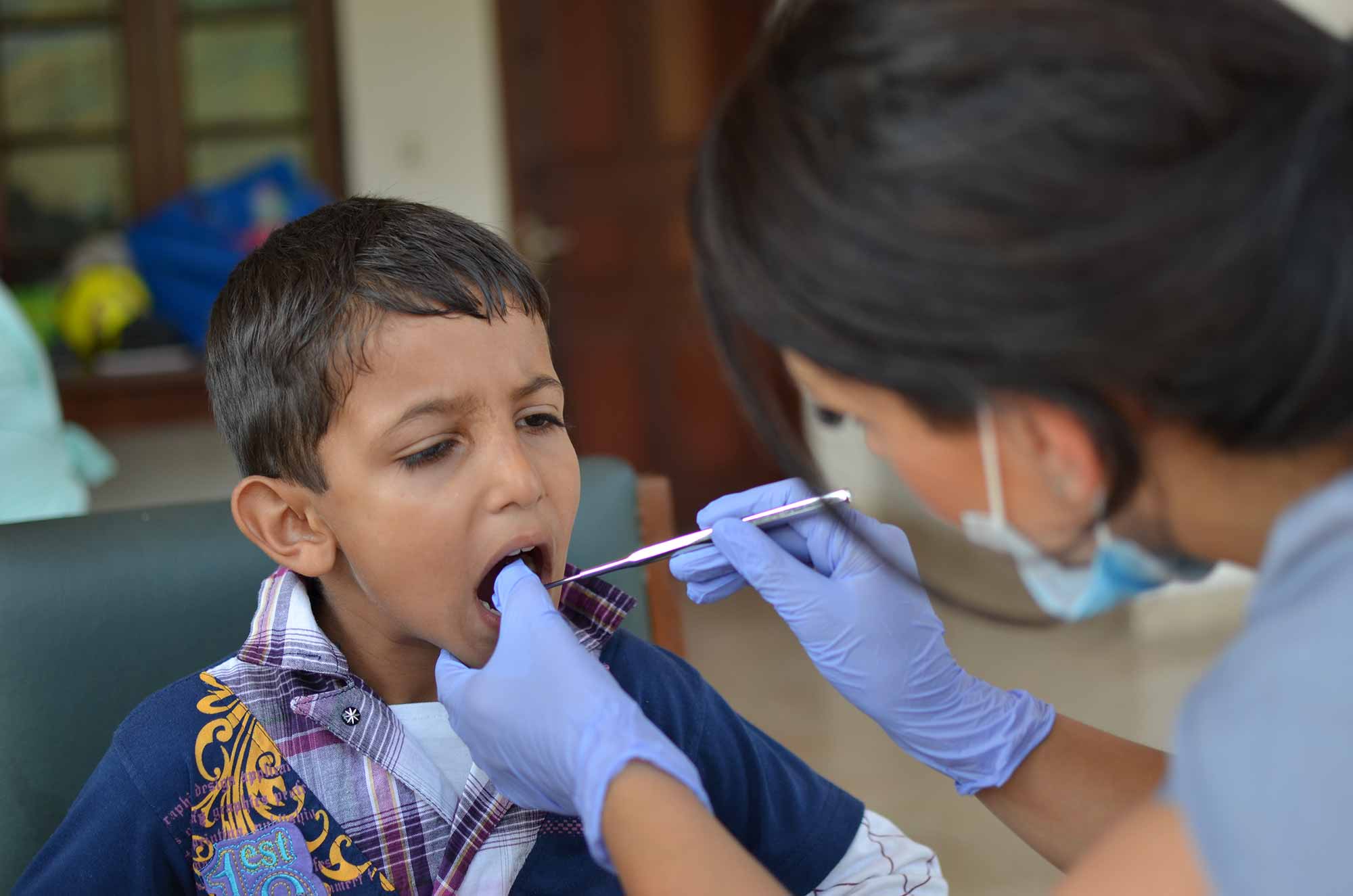 To set up a service similar to that in the UK, I would need to raise more than £30,000. We organised a charity meal and managed to raise the funds we needed.
To set up a service similar to that in the UK, I would need to raise more than £30,000. We organised a charity meal and managed to raise the funds we needed.
After purchasing two dental chairs from the UK with other small equipment and consumables required, we found local suppliers and a local engineer to install the surgeries. We commissioned the cabinetry to be made and a sterilisation room installed.
Additionally, there’s an incinerator onsite to dispose of all clinical waste. I have ensured that sterilisation procedures comply with UK standards to protect patients, staff and volunteers from spreading diseases.
New surgeries
We have provided jobs for two local dentists and two local nurses. They have had access to online training to have a better understanding of how dentistry is practised in the UK and to ensure standards of clinical practice are kept high.
Our aim is to send monthly volunteers to help support the department. They provide training and mentoring for the local dentists and nurses. We hope they will crowdfund on our behalf to support the charity’s work and help me to fulfil my obligation to maintain the department and pay the salaries to the staff.
We are also developing maxillofacial department and will be able to offer oral cancer screening. Oral cancer is the fourth most prevalent cancer and is largely preventable with education.
And in September, we will be starting cleft lip and palate surgery. We will be combining preventative and restorative dentistry with orthodontics and oral surgery. This will provide part of a multidisciplinary to treat cleft lip and palate and, once again, is based on the NHS model.
 Impact of COVID
Impact of COVID
Since the pandemic, the hospital facility stopped all elective work and prepared to receive COVID patients. We have several ventilators and extra PPE. We conducted training specific to the virus for the staff and education for the locals in the area. This includes hand washing techniques and how to stay safe with social distancing measures.
We had to cancel the trips of four volunteers due to travel in March and April. But we’re hoping to reschedule their visits next year.
We have made developments with our cleft lip and palate programme. We have a multidisciplinary team together raring to go once things settle.
This team includes an orthodontist, oral surgeon, general dentists, plastic surgeon, anaesthetist, nurses and speech therapist to enable us to achieve the best long term outcomes.
We are still keeping a close eye on government advice before reopening dental services.
Follow Dentistry Online on Instagram to keep up with all the latest dental news and trends.


