Follow Dentistry.co.uk on Instagram to keep up with all the latest dental news and trends.
 The impact of COVID-19 has been felt across the world. From dentistry to hairdressing, every profession has been affected. We hear from dentists around the world who tell us their story about how COVID-19 has affected them.
The impact of COVID-19 has been felt across the world. From dentistry to hairdressing, every profession has been affected. We hear from dentists around the world who tell us their story about how COVID-19 has affected them.
Croatia – Berislav Mostarac

In January and February 2020, many considered the coronavirus a joke. Two months later, the COVID issue became very serious.
COVID-19 devastated Italy – Croatia’s first neighbour country. The news showed death stories each day. And we, in Croatia, decided to try and win the fight against COVID-19.
Croatia closed borders and no longer welcomed travellers. The government didn’t even allow daily migrations from one city to another. Only people working for necessary government offices (health, army) could move.
Public transport stopped for almost two months. Children took online classes for three months. All institutions were on standby.
In the dental practice
In March 2020, I remember one of my patients from Ireland cancelling an already-paid full mouth rehabilitation because of unclear travelling options.
My clinic is not dental tourism oriented. But I can imagine the financial influence of COVID in other Croatian clinics specialised only for dental tourism.
Also, many clinics market towards Italian people. Thousands of people from the dental tourism industry were in trouble.
In April 2020, all dentistry was in total lockdown. The government forbid all work in dental clinics. But we had an obligation to be available for our patients via phone, video call or email.
We took advantage of the time to reorganise our business and clinic. We digitalised almost all of our papers. It was a time of non-dental but clinic management work. Urgent patients were also referred to one central office specialised and equipped for COVID-19; and we postponed all other treatments.
Public health system institutions organised three urgent offices for 900,000 people. They accepted patients with pain or swellings.
All employees of the public health system worked periodically. So a team worked a full shift every two weeks.
Patients had available dental care from 8am to 8pm. They weren’t charged for treatment. Our public health insurance company therefore paid for all treatments.
Reopening
May 2020 started with a new view on dentistry.
The Ministry of Health published instructions and protocols for safe work in this new situation. Only one patient could visit the clinic at a time. Patients couldn’t meet each other in the waiting room. Body temperature was measured before entering the clinic. Hand washing and disinfection became a standard.
We removed all necessary equipment from our clinic and implemented air disinfection systems. The patients’ mouths were always disinfected. We also worked only with suction.
As a surgery clinic we only upgraded each treatment to normal surgery treatment. And yes, our costs (masks and suites) for dental treatment were 10 times higher.
In our office we decided not to charge our patients for that. But the future will probably bring that issue into dental discussion.
A decrease in financial income, loss of foreign patients, shortage of money for employees were reasons why almost all clinics accepted costs as business costs. We were all happy to work again.
What does the future look like?
In June 2020 Croatia was a COVID-free country. We therefore started relaxing our measures.
It was a slow start, but we did the best we could to work as much as possible in two shifts. Also, two months of pause gave us economic motivation.
July 2020 I would say patients put their health in first place, even before properties and cars. We never had so much interest for full rehabilitation. Maybe patients are preparing themselves for a COVID-19 second wave.
As an aesthetic dentist, I can see nothing will stop patients from searching for aesthetic dental treatments. It therefore seems Croatian people decided to live with COVID and stay beautiful.
Today, in August 2020 we are thinking of ways to fight against COVID-19. It seems nobody is sure what the future brings.
There is an increase in the number of COVID-19 cases due to the tourist season. Some borders will close again.
We are expecting a vaccine, controlling symptoms of disease, putting our patient’s safety first. We also expect victory, our dental clinic is a place where we strongly focus on this goal.
What I can say at the end is – we must read the most recent articles and care for our patients as we care for our family. Good luck to all of us and stay safe!
Netherlands – Christine Silaghi

I am a female dentist working in Rijswijk in the Netherlands. I work as an associate and have done since 2008.
When I heard first about COVID-19 on the radio in December 2019, we were chatting at the practice with my assistant Leyla. I was complaining that our practice has been sold to a corporate. I remember Leyla saying: ‘You should not worry about that anymore. There are worse things waiting for us in 2020, like health issues’. We didn’t really take it seriously.
For every month that passed, COVID-19 came closer.
Lockdown
By 12 March, Prime Minister Rutte announced the national lockdown.
The following weeks were very quiet. The practice remained empty even though acute pain and emergences complaints were possible to treat. People stayed away from the dentist.
Staff split up in shifts to avoid contact with each other. We cleared the waiting room by removing the table and splitting up the chairs, removing magazines, newspapers and toys. We separated reception with a plastic shield.
The National Institute for Public Health updated us daily about PPE and adjusted protocols. Such as not to do surgical extractions and treatments that create a high amount of aerosols.
Our total turnover dropped every day until eventually reaching zero.
Treating patients cost us money during lockdown. The practice cancelled all regular treatments because we did not have any idea how long lockdown would go on for.
After four weeks we hoped to start again. But the government extended lockdown by two more weeks. Finally on 22 April, dentists got permission to reopen for regular treatments.
Reopening after lockdown
The first week after lockdown was quiet. Every week after that our bookings got busier and busier.
People started to gather faith and were booking appointments.
We adjusted our PPE with protective shields and placed an alcohol dispenser in the waiting room. The receptionists call all patients two days prior to their appointments. They work through triage questions.
If people have symptoms of a cold, or have had contact with people that have symptoms, we cancel the appointment and reschedule in three weeks.
In general, I can say that triaging patients has caused us more administrative work.
We now schedule extra time to let aerosols settle between appointments. Patients rinse with hydrogen peroxide 1% for one minute before entering the treatment room. And patients wait outside the building to avoid contact between appointments before calling them straight through to the treatment room.
This extra time needed is creating a 30% fall in turnover.
Wearing face shields and FFP2 masks causes us discomfort too – causing headaches and difficulties breathing. Not to mention the extra money wasted on PPE due to companies selling products at abnormally high prices.
After around four weeks I reached my original turnover again. Many people have tired of social distancing and started coming back.
The practice appointments look like normal now and we’re having to work three times harder to keep up. There’s more administration and we have to be much more efficient with treatment times, which are shortened.
UAE – Maysoon Abdelmajeed

Just as was the case globally, the UAE implemented a national lockdown in response to COVID-19.
This has had a number of significant effects on dentistry as clinical organisations scurried to salvage what they can within the limitations.
Clinical staff and environment
Initially, most dental clinics closed. This was following guidance released by the Ministry of Health that all non-urgent dental treatment must cease, and AGPs are to be avoided unless absolutely necessary.
As SOPs were re-written, clinical staff wore fully-enhanced PPE. This included long-sleeved gowns, aprons, hats, shoe covers and face shields. In addition, N95 or KN95 respirators replaced surgical masks for all members of the clinical team.
Many ignored fit testing guidance from the Ministry of Health for N95 respirators. The UAE does not have the same obligation placed on employers in the UK through the Health and Safety Act 1974.
The message of the importance of respiratory protection simply did not get through. Clinical staff carried on wearing N95 respirators not fit-tested.
There are many fake respirators in circulation. Awareness amongst the profession on this matter remains relatively low.
Dismayed at what I was hearing, I decided to start my own fit-testing service here making myself available to at least those interested.
Patient management
Sensible changes in the wider aspects of dental service delivery became commonplace.
In our practice, patients now follow a strict pathway. We check them for pyrexia on arrival and follow sign-posted distancing measures throughout their attendance.
Hand sanitisation is supervised before patients move to the reception area. Here, they stand a safe two-metre distance from the desk according to clear floor markings.
We arrange staggered appointments in an attempt to minimise patients meeting each other in the waiting room. If they do, seating arrangements mean patients sit a safe distance from each other.
UAE strongly implements laws regarding the wearing of face coverings in any public place with heavy fines. Patients therefore need no encouragement in this regard.
All surfaces in communal areas are continually wiped and we remove any potentially hazardous material such as magazines, toys and coffee cups.
With remote triaging, we carefully plan the patient’s clinical need before delivering the treatment in practice.
There is no difference in the way we manage AGPs and non-AGPs. Clinical staff wear full, enhanced PPE for both.
Rinsing with oxidising mouthwash is another additional measure for risk mitigation.
We have fallow times of 20 minutes, a protocol not arisen from any particular evidence-based guidance.
Patients’ perceptions
Generally, most patients are understanding throughout the difficult circumstances. They are happy to differ their appointments.
However, we found orthodontic patients mid-treatment were more impatient and demanding when wanting to see the dentist.
Easing of the lockdown
An interesting observation has been the effect of the travel restrictions on the number of patients we see.
July and August are notoriously quiet in the UAE. Expatriate families take their annual leave to visit their home countries. Due to travel restrictions, the summer months seem not as quiet as previous years.
Anecdotally, a few patients report spending more time working from home and attending non-stop Zoom meetings has made them more appearance-conscious. This is pushing them to seek advice for cosmetic dentistry as well as facial aesthetics.
Because the population here is largely made up of expatriates on employment visas, there are many stories of redundancies leading to repatriations. This has a somewhat interesting ripple effect. Patients rush in to have any dental treatment before employers withdraw any medical insurance policies.
Fiscal difficulties
There is no financial help through governmental support schemes available. So all businesses suffered drastically during the lockdown.
Most staff members must take unpaid leave.
Conclusion
As life changes across all sectors and industries, dentistry is no exception.
There is no state-funded service here. So the profession is entirely dependant on the self-funding or employer-insured system. We wait with bated breath to see if a global recession has an impact on the dental patient.
In the meantime, the patient and the profession at large are patiently innovating as we all adapt to the new normal.
Things are ticking over, but nobody knows, or dares to even guess, what 2021 will bring.
Denmark – Eddie Basson

The Danish government decided to close down the country on the 12 March due to the COVID-19.
For the dentists that meant sending home almost 10,000 employees. The approximately 1,800 practices were more or less closed. We were only allowed to treat the most acute patients.
Initially we where told to close down for at least three months, but that was later changed to the end of April (so a total of approximately six weeks).
Due to changing the pandemic law (from 1905) on the 12 March, with effect from the 17 March, the COVID-19 had a huge economic impact on self-employed businesses. So far at least six dental practices have closed due to bankruptcy. Some suggest we haven’t yet seen the full consequence.
What has the recovery been like?
Just because we are open again, doesn’t mean that we are back to normal.
Although dental staff work with NIR (national infection guidelines), and work at a high hygienic level, we received lots of new guidelines that didn’t necessarily make sense. But as law-abiding citizens, we follow the guidelines, and wait for the storm to pass.
For some, the guidelines look like they have been made on a desk, without adjusting it to the real world.
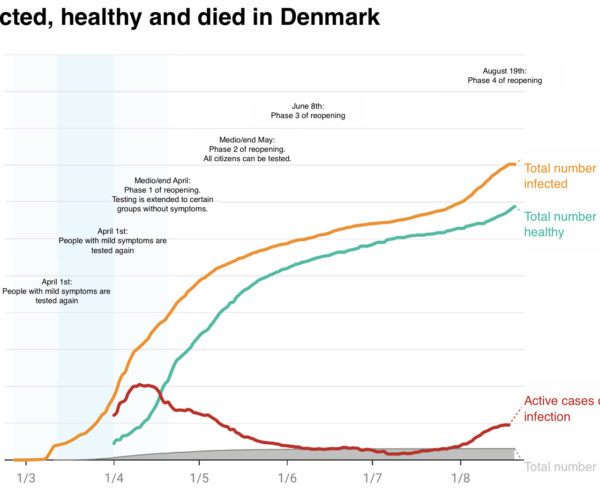
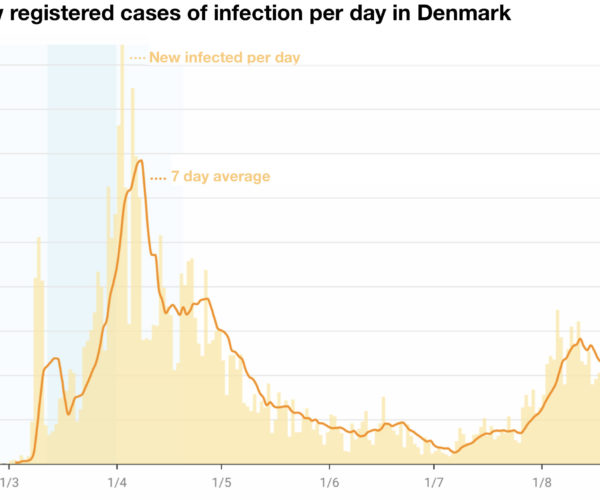
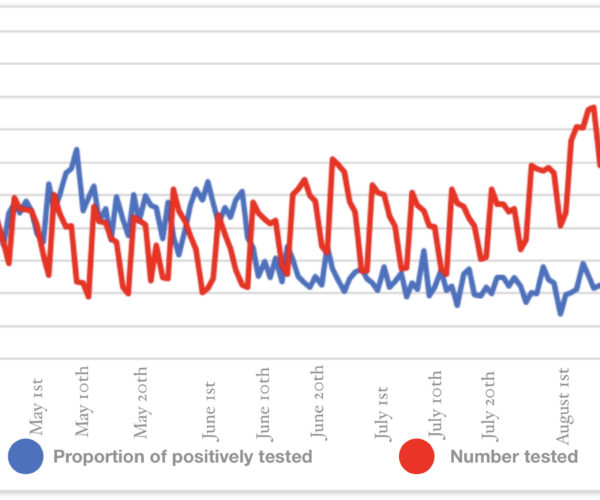
The number infected has been very low throughout the period. Although we are experiencing some rise in numbers lately in a specific area. But, on the other hand, the number of tests is also increasing quite significantly.
In the beginning the test capacity was very poor. Therefore, 230 dental practices got together offering their help testing citizens. So far the government hasn’t reacted to this proposal.
What the future might hold
Like every other event that we face, it leaves a mark. How deep this one is, I’m not sure.
A part of me hoped the startup would be slower, and hence give every practice the time and possibility to think their workflow through. Time to find how we can bring dentistry up to the next level in regards of quality and service.
But as it is now, I see practices throughout the country working faster than ever, because of the great workload that has accumulated.
Teeth have unfortunately not got any better during the past month. So there is a lot to take care of.
In regards to how we run practices, I believe this pandemic will change views on being self employed or not, unfortunately!
Small businesses are of course more vulnerable than bigger businesses. On the other hand, having more employees is a major expense with regards to salaries. The Danish government has not covered it all.
So, what to do? Well for most clinic owners, enrolling in a dental chain might seem like a natural solution. And yes, the big corporation might need to cover the majority of the loss. But remember that no one does it for free. We will need to pay the losses back.
USA – Chris Bowman

If you were to tell me in January 2020 that I would temporarily close my thriving dental practice in Charlotte, NC just three months later because of a global pandemic, I would have laughed you out of the room!
But as we all now know, the COVID-19 virus began to spread like wildfire around the world.
Along with it came uncertainty, confusion, and a deep concern for doing everything we can to keep others healthy, safe, and even alive.
Closing the practice
After learning about the emerging COVID-19 pandemic, I made the difficult and painful decision on 23 March to temporarily close my practice. With the exception of dental emergencies.
State dental boards and national associations around the US were advising all dentists to do the same. And virtually all dentists did.
My administrative team worked full time to cancel appointments and place patients on our priority reappointment list. I reluctantly furloughed almost all of my clinical team, including myself!
Even though I was seeing some patients for emergencies, I took no salary during the six weeks we were shut down.
My goals and objectives during the temporary closure of my practice were to stay in touch with my patients. And to prepare my practice for a safe reopening at the right time.
I also helped my team acquire the appropriate unemployment benefits. And stayed in close contact with my bankers and accountant regarding newly available funding for small businesses.
Finally, I began my quest to acquire sufficient PPE and other safety equipment for my practice. That was perhaps the most challenging chore!
Needless to say, keeping up with all of the above was a full-time job itself. I found myself working longer hours than when I actually see patients.
Delivering safe dental care
I set out to make my practice the safest environment to deliver and receive dental care possible.
In addition to our extensive PPE inventory, I acquired eight HEPA-13 air filters, which remove viruses from our air. I also installed an industrial ozone generator with UV-C light. This runs automatically at the end of each workday after everyone has left.
We then added two low-volume disinfectant foggers, which we use at least twice daily in treatment rooms. The electrolyzed saline (hypochlorous acid) we use is 200 times more powerful than bleach, but safe enough to wash fresh fruits and vegetables at grocery stores.
Finally, we now infuse our operatory water with ozone gas. This makes our water viricidal and bactericidal. So the very aerosols we generate while treating patients are instantly neutralised.
Adding these amenities to my practice has given our patients extremely high levels of confidence. A virus doesn’t stand a chance here!
Reopening
I’m so appreciative of my team during this whole pandemic for their unique efforts and dedication to keeping us all safe and healthy, and busy!
We reopened after six weeks of almost complete closure.
Reactions from our patients have been outstanding. They are relieved and excited that their dentist has reopened safely. But they also comment frequently about how confident they feel in my practice.
We kept them informed of our progress and innovations during the six-week closure period. I credit that frequent communication with our ability to relaunch safely and hit full capacity quickly.
Our current monthly production and revenue numbers are now higher than the same months in 2019.
A true leader
As we continue to learn more about the events surrounding COVID-19, we realise the opportunities we have to make our practices better.
I believe dental practices around the world can now be safer for patients, and themselves. The attention we pay to patients and team members through positive and proactive communication will pay off huge through increased confidence, loyalty, and ultimately increased business and referrals.
By recognising how you can make a bigger difference for your patients and your community, you can stand out as a true leader while many around you are looking for answers for their oral health!
With thanks to Jan Einfeldt for all his help with this article.